
UVGI lights for 15 minutes, wet oven heat for 30 minutes, also as effective in eliminating viruses on N95 masks, potentially offering an immediate health worker remedy
An Air Force report from 2012 shows how to sterilize N95 masks using hot steam from microwave and standard ovens, as well ultraviolet germicidal irradiation (UVGI) light bulbs. The success rate was 93 percent with all three methods.
Healthcare workers on the front lines of treating patients with novel coronavirus (COVID-19) are at high risk of contracting the disease themselves, in part because a shortage of N95 masks has forced them to reuse contaminated masks that would otherwise be swapped out between patients. The inexpensive techniques outlined in the Air Force report could help provide critical protection to workers, nurses, doctors and support staff tackling the 2020 COVID-19 pandemic.
Medical volunteers, who have stepped forward by the thousands across the U.S., could also apply the methods used in the Air Force report (highlighted by EnviroReporter.com) to arm America’s frontline medical warriors with the virus-free N95 masks they need to save lives.

“A major concern among healthcare experts is a projected shortage of N95 filtering facepiece respirators (FFRs) during an influenza pandemic,” the June 12, 2012 report said. The lead author of the document was Brian K. Heimbuch for Applied Research Associates, the lead subcontractor. “One option for mitigating an FFR shortage is to decontaminate and reuse the devices.”
“The focus of this research effort was to evaluate the ability of microwave/steam energy, low-temperature moist heat, and ultraviolet germicidal irradiation at 254 nm to decontaminate H1N1 influenza virus loaded onto FFRs as either aerosols or droplets,” the study abstract continued. “Our data indicate that all three decontamination technologies provide > 4-log reduction of viable H1N1 virus –in 93% of our experiments, the virus was removed to levels below the method detection limit. These data are encouraging and may contribute to the evolution of effective strategies for decontamination and reuse of FFRs.”
While this peer-reviewed report proposed relatively simple solutions to one of the pandemic’s most vexing problems – keeping the medical corps protected by plenty of clean N95 facemasks – its very promise begs the question: Why hasn’t this game-changing information, already approved by the Centers for Disease Control (CDC) – including as a COVID-19 “crisis standards of care” recommendation – been made widely available during the current COVID-19 crisis?
It’s a stretch to believe that the U.S. Air Force, or the study’s authors, could forget a report paid for with taxpayer dollars that demonstrates simple ways to protect our medical frontline with common equipment still available online.
STERILIZATION SOLUTIONS
The June 2012 Air Force Research Laboratory study from Tyndall Air Force Base in Florida was called “A pandemic influenza preparedness study: Use of energetic methods to decontaminate filtering facepiece respirators contaminated with H1N1 aerosols and droplets.”
The 11-page paper showed that a simple microwave energy steam process takes just two minutes and has a 93% success rate in leaving no trace of the test virus on FFRs. A repeat of the procedure could bring that success rate closer to 100%.
“The biocidal activity of microwave energy has been well documented; however, moisture is a key factor, given that microwaves are considered by some to be nonbiocidal,” the report said. “Accordingly, the FFR was positioned above an improvised water reservoir during decontamination (Fig 1A). Steam produced from microwave heating of the water is the primary means of biocidal activity.”
The N95 masks were placed singly in a typical 1250-watt microwave oven by balancing the FFR on top of two microwave-safe plastic containers with a couple of ounces of warm water covered by lids with holes for the steam to escape upwards through. Heimbuch and associates then set the microwave on high for two minutes and, in 93% of the time, the result was a sterilized mask with no trace of virus.
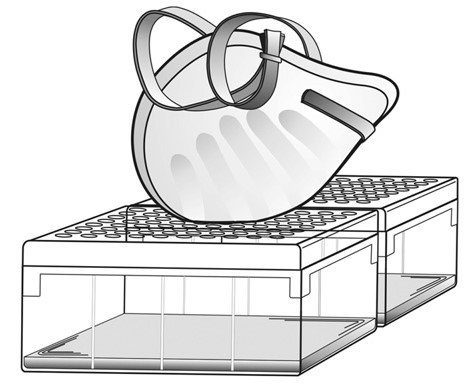
While metal objects generally should not be used in a microwave oven, the study found that no arcing was observed from the N95 mask, which has a thin metal nose clip and four small staples affixing the elastic head bands. The study also noted that the masks weren’t significantly deformed in the microwave process. The result is an FFR that can potentially be reused at least 5 to 20 times when well cared for, as EnviroReporter.com‘s years of experience with the masks can attest.
This technique, while simple, is best applied in a medical setting where dedicated microwaves could be used for the sterilization. For normal folks with FFRs, the process is a riskier endeavor due to the potential for errors in the steaming/heating/microwaving of N95 masks.
That said, people dealing with a COVID-19 victim(s) in their own home could help maintain strict viral protection for the patient’s caregiver(s) by using this technique in an emergency, provided the microwave becomes only used for sterilization to prevent possible cross contamination with heated food and drink.
“The initial reports showed microwaves to be an effective microbicide,” says the current CDC Other Sterilization Methods. “The microwaves produced by a “home-type” microwave oven (2.45 GHz) completely inactivate bacterial cultures, mycobacteria, viruses, and G. stearothermophilus spores within 60 seconds to 5 minutes depending on the challenge organism. Another study confirmed these results but also found that higher power microwaves in the presence of water may be needed for sterilization. Complete destruction of Mycobacterium bovis was obtained with 4 minutes of microwave exposure (600W, 2450 MHz).”
Microwaves are affordable and commonly twice the power at 1,250W (watts) than the one used by the CDC to get “complete destruction” in four minutes. Over 13 million microwaves were sold in America last year and almost every single one of them can sterilize an N95 mask. Two minutes to four minutes a mask. In and out.
Americans could ‘gift’ medical clinics in their areas with microwaves in a coordinated campaign to equip any and all facilities that deal with the novel coronavirus with adequate new microwaves for sterilization. Volunteers could be trained to crank out cleaned masks as well.
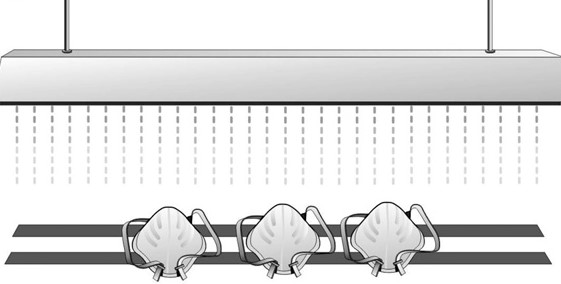
Already, states like Massachusetts and California are investing big time in machines that use hydrogen peroxide vapor to sterilize 80,000 N95 masks per day. Alternative sterilization solutions could also include ultraviolet light devices, such as this $60 ultraviolet germicidal irradiation lamp in a light with aluminum reflector that, after 15 minutes four inches off the N95s, has FFRs virus-free with the same stunning 93 percent success rate.
The Air Force report has diagrams, shown here, that detail each of these deceptively simple techniques including heating up water in a conventional oven to generate “warm moist heat” or WMH. The WMH setup has the FFRs in an oven-proof container with water in it heated for three hours to create steam. Add the mask for 30 minutes and you kill the viruses below detectable limits 93 percent of the time.
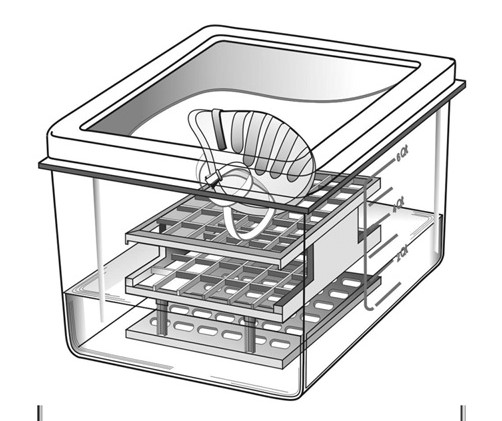
Heimbuch and Applied Research Associates knew they were onto something good when they created this report for the Air Force in 2012. Their analysis led them to favor the microwave generated steam as “the least time-intensive method and requires only a simple FFR holder/water reservoir. The simplicity of the technique and the ready availability of microwave ovens favor this technology for use in the home and by small organizations.”
“Although UVGI is the least invasive of the 3 methods and is readily scalable to meet the needs of larger organizations, it relies on a hazardous light source, which might be prohibited for home use,” the study continued. “However, the cost of the device could be easily absorbed by most organizations even if multiple UVGI sources are needed to meet their demand. Many types of UVGI systems are currently used in hospitals for air purification, biological safety cabinets, and surface sterilization. Adapting such systems for decontamination and reuse of FFRs could be a low-cost option for hospitals, and organizations purchasing UVGI systems for other applications might want to select designs that can be used for decontamination of FFRs as well.”
“The ideal FFR decontamination technology will preserve performance and fit, leave no
residual toxicity, and be fast-acting, inexpensive, and readily available,” Heimbuch wrote in 2012 for the Air Force. “[W]e are optimistic that our evaluation of these energetic methods may help lead to solutions to mitigate a shortage of FFRs caused by pandemic influenza.”
“IF THE PANDEMIC WOULD HAVE HAPPENED NEXT YEAR”
That was in June 2012. But in the midst of the pandemic in the United States in April 2020, there has been no Air Force coming to the rescue telling us that it already knows how to sterilize those critical N95 masks worth their weight in gold with oven or microwave steam. Or that hospitals may already have enough UVGI lamps throughout their facilities performing various functions that could be repurposed to sanitize FFRs or that such lamps are available online.
Heimbuch, who cited six reports that he either authored or was a part of in the references for his 2012 Air Force-funded N95 mask report by Applied Research Associates, did say something about FFRs in a recent MSN article April 3 republished from the Washington Post, called “Federal government spent millions to ramp up mask readiness, but that isn’t helping now.”
The article states that “[T]he Trump administration contracted with Applied Research Associates of Albuquerque to create a prototype of a ‘next-generation respirator’ as the masks are called, that could be sanitized and reused during public health emergencies” and that Applied Research Associates was awarded $4.8 million for the project, but the deal “came too late for the coronavirus outbreak.”
Heimbuch is quoted, saying: “Unfortunately, if the pandemic would have happened next year, we’d have been in much better shape.”
He doesn’t mention his own 2012 study for the Air Force, which demonstrates that the current generation of N95 masks don’t need millions in rethinking – they can be sterilized with microwave ovens, UVGI lamps and warm moist heat.
Not next year. Now.












Your article will surely help many people, thanks for sharing!
Covid-19 is a disaster for the whole world, may all come through it safely.
The Science Times reports on the N95 sterilization process first reported by EnviroReporter.com here. [https://www.sciencetimes.com/articles/26405/20200710/sterilizing-n95-masks-microwave-effective-heres-sterilize.htm]
“The Air Force reported way back in 2012 how to sterilize N95 masks using hot steam from microwave and standard ovens, and also the using the ultraviolet germicidal radiation (UVGI) light bulbs. It is an inexpensive technique that can help provide critical protection to frontline workers.”
The article includes a superb video showing a doctor using the technique safely. [https://youtu.be/2K58GONdWh8]. He says that the reason the metal clip in the nose part of the N95 mask doesn’t arc is because it is covered completely by fabric, a factoid we were previously unaware of. The doctor shows that with 7 ounces of water, the proper setup, and 4 minutes in a typical microwave oven, sterilizes 4 masks at a time, leaving them perfectly dry to the touch after processing.
It is gratifying to see this information reported by EnviroReporter.com being utilized by our frontline medical heroes. Their message to you, as is ours, mask up or be a deplorable maskhole. [https://www.urbandictionary.com/define.php?term=Maskhole]
This an awesome article. Thank you so much for putting the power to sanitize N95s in all our hands. This needs to be shared and used.
Some protection is still better than no protection. Even if reduces infectivity by 30%, just by acting as a barrier for droplet transmission, it’s a worthy precaution to embrace.
Thank you for this timely article giving us important information on N95 mask sterilization. I think (only my opinion) this would also apply to other types of non-N95 thinner surgical mask face coverings which are too delicate to wash in the laundry. Washing cloth face coverings is the method recommended for cleaning more durable face coverings.
I am always concerned when government elects NOT to give us information that they already have available. Likely, they do not wish to encourage the general public to seek out N95 masks which might deprive front line medical providers of this limited resource. Some of us have a few masks, bought years ago for potential radiological hazards dicussed In many articles on this website over the years. Our limited household supplies need to be conserved by allowing reuse with cleaning methods such as the ones discussed above.
Importantly, if you have valved N95 masks, they may offer the wearer some protection against getting viruses, but if you have the virus it will not protect those around you from getting the virus from you. The filtering action of valved N95 masks is one-way, and would not be as useful in mixed healthy/infected environments. Often, as many as 50% of infected individuals display no symptoms, and do not know they might be spreading the virus. Such as person wearing a valved N95 mask would not be protecting healthy individuals around them.